In vitro fertilization(IVF) cycles usually allow a higher number of eggs to be retrieved from the ovaries. Those that are mature are fertilised with sperm a few hours after they are removed from the ovary and then cultured by embryologists in special incubators. If fertilisation takes place as it should, from the next day onwards we no longer talk about an egg, but about an embryo. “Most patients assume that out of all the eggs collected we will have a suitable embryo for transfer to the uterus,” says doc. Dr. Silvia Toporcerová, PhD, Medical Director of the Gyncare Centre and adds: “This is unfortunately not true. Both egg and sperm have biological limitations, and not everyone will produce a healthy embryo. Some of the eggs are not suitable for fertilization, some of those suitable eggs do not fertilize, a large proportion of the embryos stop dividing during the first five days in our laboratory and are not suitable for transfer. It is a completely natural phenomenon. Anyway, at the moment when the embryo is completed to the stage of an expanded blastocyst, and this is 5. – On the 6th day after fertilization, it must either be transferred to the uterus or frozen. From this stage onwards, it needs the environment of the uterus for further development.”
Currently, most IVF cycles involve prolonged embryo culture to 5. – On the 6th. If the patient couple has several suitable embryos for transfer into the uterus on that day, the most promising embryo should be selected. Today, there are a number of special methods for this, but the basic one used in every single case is their morphological assessment – that is, the assessment of the quantity, shape and regularity of the cells.
On the fifth day, the embryos develop to the blastocyst stage
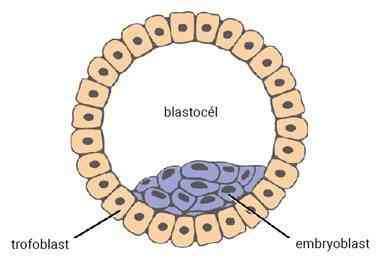
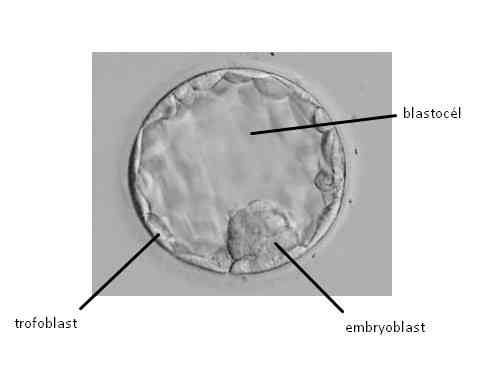
At the embryonic blastocyst stage, the cells of the embryo are already divided into the embryoblast (inner cell mass – ICM), which gives rise to the embryo itself, and the trophoectoderm – trophoblast, which develops into the placenta and amniotic membranes. Inside the blastocyst is a cavity filled with fluid called the blastocele.
Gardner rating system
Currently, the most widely used system for morphological evaluation of blastocysts is the Gardner grading system. Morphological assessment means that each blastocyst is categorised according to how its individual components – embryoblast, trophoectoderm and blastocoel – look under the microscope.
Gardner’s rating system consists of three characters – the first is a number, the second and the third is a letter.
- The first character in the system is a digit from 1 to 6, which basically indicates the size and expansion of the blastocyst (expansion means the relative volume of the blastocyst to the size of the blastocyst).
- The second character is the letter A, B or C, which indicates the morphological quality of the embryoblast.
- The third character is the letter A, B or C, which indicates the morphological quality of the trophoectoderm.
Thus, the best quality blastocysts have the designation 6AA, 5AA, or at an earlier stage 4AA.
What do the different numerical stages of development indicate?
- An early blastocyst in which the cavity has just begun to form – the blastocyst is less than half the volume of the embryo.
- A blastocyst in which the blastocyst occupies more than half the volume of the embryo.
- A full blastocyst in which the blastocyst completely fills the entire volume of the embryo.
- The expanded blastocyst, which is already significantly increasing its total volume, the blastocyst completely fills the embryo and the embryo envelope (zona pellucida) gradually becomes thinner.
- Hatching blastocyst whose envelope (zona pellucida) ruptures with further volume growth and some trophoectoderm cells move outside it.
- A hatched blastocyst (hatched blastocyst) that has completely left the envelope (zona pellucida) and is ready to nest in the uterine lining.
Assessment of cell mass (ICM)
- A – numerous cells, regularly arranged.
- B – less numerous cells, loosely clustered.
- C – very few loosely clustered cells.
Trophectoderm status designation
- A – trophectoderm is formed by regular cells that form a cohesive layer.
- B – large less numerous cells, irregularly arranged.
- C – very few large irregular cells.
By evaluating these three components, embryologists combine the three traits to indicate the morphological quality of each blastocyst evaluated. The use of Gardner’s system is beneficial mainly because a strict morphological evaluation minimizes the degree of subjectivity – that is, the subjective view of each individual embryologist who sees the embryo under the microscope. The score provides an accurate assessment – a description of the quality of the individual parts of the blastocyst. Of course, the experience of the embryology assessment team also plays an important role in this assessment.
Practical examples of the evaluation of individual blastocysts
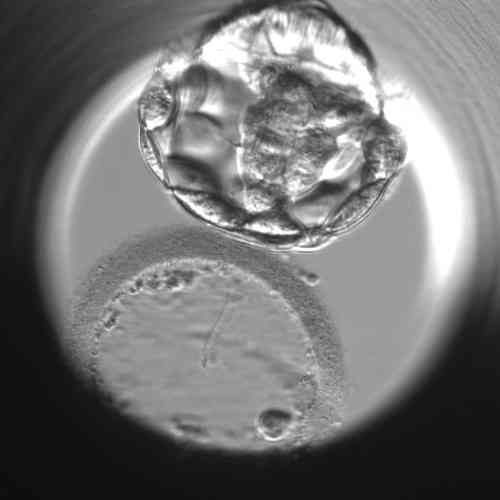
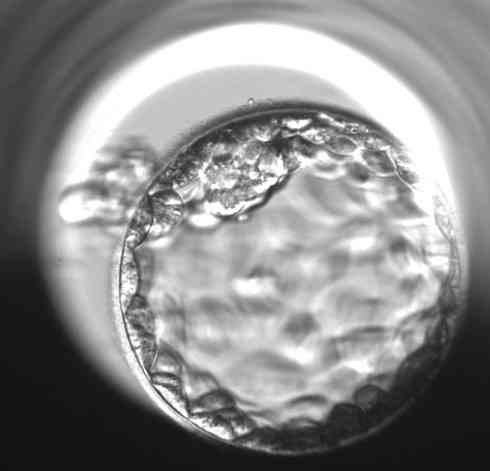
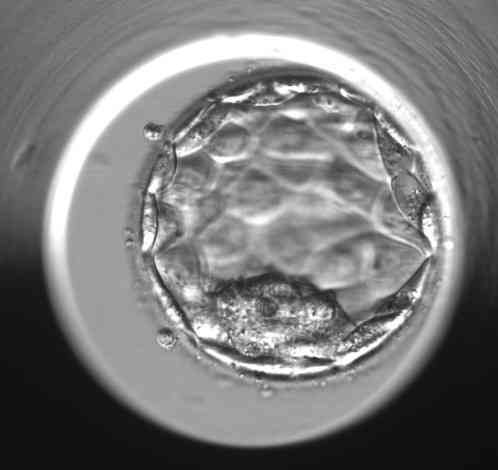
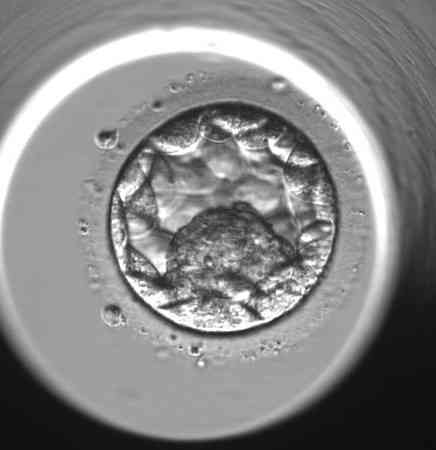


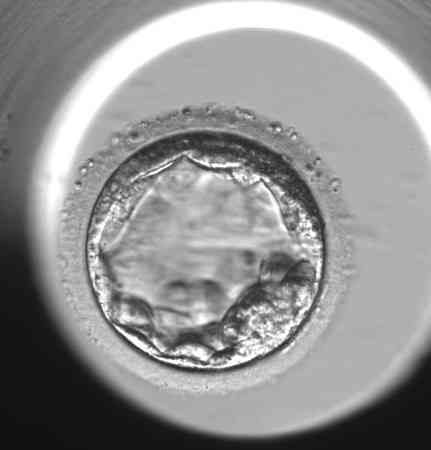
“However, the morphological evaluation of the blastocyst is always only one part of the whole puzzle of information that will help us to select the most promising embryo for transfer into the uterus,” says Bc. Dominika Remešová, Dis., senior embryologist at the Gyncare centre in Košice and adds: “The morphological picture of the embryo is the basis, but in addition to that, several other information we have about the embryo is important. For example, the regularity of cell division during early cell division, the temporal consistency of individual divisions, the percentage of small fragments that are produced during cell division. There are very many of these features. In the overall assessment, we are greatly assisted by so-called time-lapse monitoring, which means that a camera is placed in the special incubator where the embryos are cultured, and it takes a photograph of each embryo several times an hour. A computer puts these pictures together into a video loop that we can play around and really track the cell division in a rigorous way.” Although it is labour-intensive and takes embryologists quite a lot of time, some studies have shown that time-laps monitoring can increase the success rate of IVF by up to 8%-10%.
Given that even a shape and morphokinetically optimal embryo does not have a hundred percent probability of nesting in the uterus and developing further, a great deal of research activity in contemporary embryology is invested in efforts to improve and develop diagnostic methods that allow the selection for transfer of the most potent – the best quality embryo available to the patients in question.


