INFERTILITY TREATMENT
Diagnostics
The first step to successfully addressing fertility issues is to determine their cause. For this, we offer a wide range of reproductive health examinations for both women and men. It is important to realize that infertility is a couple’s issue, and therefore, both partners must undergo initial basic diagnostics.
We will perform the initial diagnostic examinations for you directly during the free introductory consultation. All basic initial examinations for women are covered by health insurance. The price for a basic male fertility examination – sperm analysis – starts from 30 €. If you have any examination results from your gynecologist or from previous treatment, please do not hesitate to send them to us or bring them with you to the introductory consultation.
Female Diagnostics
Ovarian reserve provides us with information about the egg supply, i.e., the number of remaining eggs (oocytes) a woman has in her ovaries. It is one of the basic indicators of a woman’s fertility level, especially important if you are planning to postpone parenthood or are having difficulty conceiving and are preparing to undergo one of the assisted reproductive methods.
The examination consists of two parts: determining the level of AMH (Anti-Müllerian Hormone) in the blood and assessing the number of follicles in the ovaries using ultrasound – AFC (Antral Follicle Count). Follicles contain immature eggs, and a higher number of them may indicate a better ovarian reserve, and vice versa. AMH levels correlate with the number of eggs in the ovaries, as it is produced by the follicles. It provides us with information about the quantity of eggs a woman can still release and is always interpreted with regard to the patient’s age. A low level may indicate reduced ovarian reserve or premature menopause.
This is a standard gynecological examination performed with an intravaginal (vaginal) or transabdominal (abdominal) probe. This examination has several applications during diagnosis and treatment. We use it to determine:
- the presence of a dominant follicle in which an egg matures, and thus confirmation of ovulation
- the height and structure of the uterine lining (endometrium), which should reach 8-12 mm at the time of ovulation (egg release)
- the number and development of follicles with eggs during hormonal stimulation
- the position of organs in the small pelvis and the position, size, and shape of the uterus, the shape of the uterine cavity, the position, size, and structure of the ovaries, the number of antral follicles (to determine egg supply)
- Monitoring Blood Flow and the Presence of the Corpus Luteum
Ultrasound examination of fallopian tube patency and uterine condition is a non-invasive procedure typically performed on an outpatient basis without anesthesia. It involves inserting a thin catheter into the uterus, through which a contrast agent visible on ultrasound is administered. During the examination, the doctor observes whether the contrast agent passes through the fallopian tubes and reaches the ovarian area.
Uterine NK cells (from Natural Killer) are a special type of immune system cells commonly found in the uterus. These cells play an important role in embryo implantation and placental development. Unlike classical NK cells in the blood, which fight infections and tumor cells, uNK cells have more of a regulatory function – they support embryo nutrition and manage immune tolerance to the fetus. In addition, they also provide basic immune protection for the uterus against pathogens. Both low and high numbers of these cells can lead to problems with embryo implantation.
This examination is performed by endometrial biopsy (sampling a part of the uterine lining) during a specific phase of the menstrual cycle, and subsequently, the number and activity of NK cells are analyzed and evaluated. We recommend performing it in cases where:
- Recurrent miscarriages have occurred
- Recurrent implantation failures have occurred after IVF
- In case of a history of preeclampsia or placental complications
If excessive uNK cell activity is detected, appropriate therapy can be chosen.
The test examines whether the endometrium is ready to receive an embryo at the correct time. During the cycle, the uterine lining changes, and there is a short period – the so-called implantation window – which is most suitable for embryo implantation. For some women, this window may be shifted, occurring earlier or later than expected. If the embryo is transferred at the wrong time, it may not implant, even if it is otherwise healthy and of good quality. The results will therefore tell us whether the endometrium is:
- Receptive – the implantation windows are at the normal time.
- Non-receptive – the implantation windows are shifted, and embryo transfer needs to be timed individually.
This test is recommended in cases of repeated embryo implantation failures during IVF, for women with a thin or abnormally developing endometrium, or for patients with a history of recurrent miscarriages.
This is an examination of cervical mucus collected after unprotected sexual intercourse. It is performed at the time of ovulation when the mucus has optimal properties for sperm penetration into the uterus. The mucus is examined immediately after collection under a microscope. Under normal circumstances, motile sperm should be present in the mucus. The number of sperm, their motility, and the quality of their movement are evaluated.
From the results, we can see the ability of sperm to penetrate the cervical mucus and survive in this environment. The absence of motile sperm may indicate a problem either on the part of the female partner (unsuitable mucus composition), the male partner (inadequate sperm motility), or it may simply indicate incorrect timing of the examination or an insufficient mucus sample.
For example, a high percentage of immotile sperm may be caused by the presence of anti-sperm antibodies, which cause their immobilization or agglutination. Agglutinations are live but prevent sperm from moving, thereby blocking the sperm’s ability to fertilize an egg.
Male Diagnostics
The basis of male diagnostics is sperm analysis. We offer several types of sperm analysis examinations with varying degrees of complexity in the parameters tested. Each of these examinations is equally simple for the patient – simply book an appointment, come to one of our clinics at the agreed time, and provide an ejaculate sample in the privacy of the collection room. Collection is performed by masturbation into a designated sterile collection container, which you will receive from us.
Reference values for normal sperm analysis according to the World Health Organization (WHO) standards are:
- Ejaculate volume: minimum 1.5 ml
- pH: 7.2 – 8.4
- Sperm concentration: minimum 15 million sperm/ml
- Total sperm motility: minimum 40%
- Number of progressively motile sperm: minimum 32%
- Number of morphologically normal sperm: minimum 4%
This is a basic examination that evaluates ejaculate quality (volume, appearance, consistency, pH, liquefaction time), as well as the presence of sperm and their characteristics or the presence of other cells.
For sperm, the following are further evaluated:
- Concentration
- Vitality
- Motility
- Morphology (shape)
In this case, the basic BASAL sperm analysis is performed using a certified CASA device for sperm analysis, utilizing artificial intelligence. This modern technology accelerates, automates, and standardizes the evaluation of individual parameters. The results also include a short video capturing your sperm.
Compared to the basic parameters included in BASAL Sperm Analysis, this sperm analysis is also extended to include genetic sperm fragmentation testing.
DNA fragmentation is an important parameter for assessing male fertility.
Due to various factors, DNA strand breaks occur, which can result in single-strand (1) or double-strand (2) breaks, depending on whether one or both strands of the DNA double helix are interrupted.
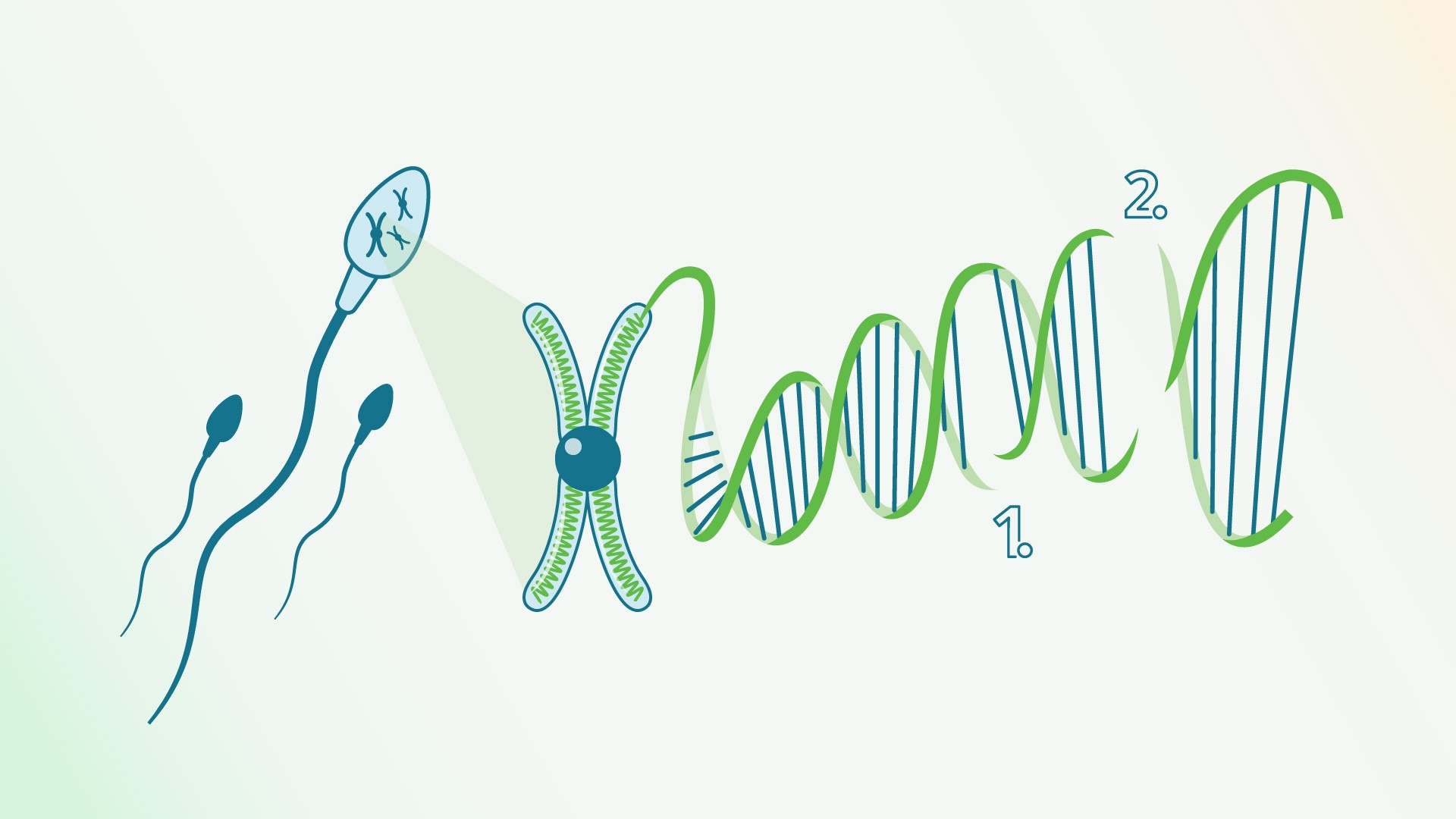
Such damage negatively affects the sperm’s ability to fertilize an egg, as well as the healthy development and division of the embryo. Embryos resulting from fertilization by sperm with such damaged DNA have slower development, which often stops before reaching the blastocyst stage.
Furthermore, men whose sperm analysis appears normal in terms of standard parameters such as sperm count, motility, and morphology may also have high DNA fragmentation.
PREMIUM Sperm Analysis is the most comprehensive sperm examination, which, in addition to basic parameters and DNA fragmentation, also examines another important indicator – oxidative stress in sperm. Oxidative stress is a condition where free radicals (reactive oxygen species) exceed the antioxidant defense capacity of seminal plasma, which can lead to DNA damage in sperm, as well as impaired sperm morphology, reduced motility, and thus reduced ability to fertilize an egg.
When should this examination be considered?
- In cases of idiopathic infertility (without an apparent cause)
- In cases of borderline or abnormal sperm analysis results
- In cases of IVF treatment failure
- In cases of poorer egg fertilization results with the ICSI method
- In cases of recurrent pregnancy loss
- In men with varicocele, infection, inflammation, or other risk factors (smoking, stress, poor diet, etc.)
A significant portion of male infertility cases is associated with oxidative stress, even in men with normal sperm analysis parameters. Detecting its presence allows for the implementation of appropriate personalized treatment, primarily based on lifestyle changes and increased antioxidant intake.
Patients insured with UNION insurance company are entitled to a one-time contribution of 100 € for PREMIUM Sperm Analysis!
In addition to sperm analysis, we also offer other diagnostic methods:
This is a special supplementary examination that visualizes antibodies bound to sperm. These antibodies present in the ejaculate cause sperm agglutination, reduce their motility, and thus decrease the chances of conception. The examination is suitable for normal to borderline sperm analysis parameters, or if sperm agglutination is confirmed during a basic examination.
The CatSper test identifies the functionality of special ion channels – CatSper – in the sperm membrane. Their activation allows sperm to effectively penetrate the egg. If these channels are non-functional, the sperm cannot penetrate the egg’s outer layers, and thus fertilization does not occur. In such a case, the ICSI method must be used for egg fertilization within IVF. Dysfunction of CatSper channels represents the most common undetected cause of male infertility.
A supplementary sperm analysis examination particularly suitable for borderline parameters of the basic sperm analysis. During the test, sperm are separated from other components of the ejaculate, isolating highly motile sperm that should be capable of fertilizing an egg. The examination helps in deciding which infertility treatment method is most suitable for the given patient.
Price list
 Download full price list in PDF
Download full price list in PDF

 Close details
Close details


